Translate this page into:
Immune Thrombocytopenia and Acute Kidney Injury in a Patient of Tuberculosis – A Rare Entity
*Corresponding author: Mayuri Ravi Mundhe, Department of Internal Medicine, Government Medical College, Nagpur, Maharashtra, India. mayu.mundhe@gmail.com
-
Received: ,
Accepted: ,
How to cite this article: Deshpande A, Mundhe MR, Deshmukh M. Immune thrombocytopenia and acute kidney injury in a patient of tuberculosis: A rare entity. Vidarbha J Intern Med 2022;32:80-2.
Abstract
Tuberculosis (TB) remains a common disease but has atypical presentations. The association of TB with immune thrombocytopenia is not well recognised. The purpose of this case report is to highlight the rare complication of immune thrombocytopenia secondary to TB in an endemic country like India. Prompt initiation of antitubercular therapy and steroids not only reduces the need for unnecessary transfusions but also hastens the recovery of the patient. Knowledge about rare presentations of TB leads to a better outcome in patient management.
Keywords
Immune thrombocytopenia
Acute kidney injury
Tuberculosis
INTRODUCTION
India is the highest tuberculosis (TB) burden country with an estimated incidence of 26.9 lakh cases in 2019 World Health Organization.[1] India accounts for about 24% of the global prevalence, 23% of the global incident cases, and 21% of the global TB deaths. TB can have a wide variety of haematological manifestations. Anaemia is the most commonly observed haematological abnormality, with the anaemia of chronic disease being the most common type.[2] On the other hand, isolated thrombocytopenia is the least common haematological manifestation. Acute kidney injury in a patient with TB can be as a result of antitubercular therapy or as a part of renal TB. Here, we describe a rare case of pulmonary TB presenting with immune thrombocytopenia and acute kidney injury.
CASE REPORT
A 16-year-old girl presented to the hospital with complaints of haematuria, bleeding per rectum, petechiae, and purpura all over the body for 2 days before admission. The patient had a 2-week history of cough with expectoration for which she was evaluated. She was diagnosed with sputum-positive TB 15 days before presentation and started on antitubercular therapy. During the hospital stay, the patient complained of decreased urine output and was anuric for 3 days and showed a decline in renal function so haemodialysis was initiated.
On admission, the patient was thin built, with a body mass index of 17 kg/m2. Blood pressure was 110/70 mmHg. The patient had pallor, petechiae all over the body and had bilateral pitting oedema feet. Respiratory system examination was suggestive of pleural effusion. Rest all systems were within normal limits.
A complete blood picture revealed severe anaemia (haemoglobin – 4 g/dl), with MCV of 67 and platelet count of 55,000 which further decreased to 14,000 on serial monitoring. The patient had a normal liver function but showed a rapid decline in renal function with rising urea and creatinine. Serum electrolytes were within normal limits. Ultrasonography was suggestive of chronic cystitis with normal kidney sizes, normal liver, and spleen. HIV status was negative so were HBsAg and HCV. Urine routine microscopy revealed proteinuria of 2+, 40–60 RBCs, and 2–3 pus cells. ANA was done to rule out thrombocytopenia as a part of connective tissue disorder and was reported negative. Coombs’ test was negative. Pleural fluid analysis revealed a blood tinged tap with haematocrits of 8%, protein of 2280, sugar of 122, and a total of 800 cells of which 60% were polymorphs and 40% were lymphocytes. Blood sugar at the time of pleural tap was 112 mg/dl. Pleural fluid CBNAAT was positive. Chest X-ray showed right-sided pleural effusion. Electrocardiogram was within normal limits. Bone marrow aspiration revealed a normocellular marrow with M:E of 1:1.5 and an increase in the number of megakaryocytes with peripheral destruction of platelets suggestive of immune thrombocytopenia. The patient was given platelet and blood transfusions were started on steroids, and according to the creatinine clearance, reno safe antitubercular therapy consisting of rifampicin in a dose of 10 mg/kg/day, isoniazid 5 mg/kg/day, pyrazinamide 30 mg/kg thrice weekly and levofloxacin 500 mg on an alternate day was initiated.[3] Platelet count increased to 80,000 per microlitre after 1 week and reached above 150,000 per microlitre after 2 weeks of the antitubercular therapy and prednisone. There were no fresh bleeding from any sites and no new petechiae and purpura. The patient initially responded to treatment but suddenly became dyspnoeic then landed in sudden cardiac arrest and succumbed.
DISCUSSION
TB is associated with a variety of haematological abnormalities such as anaemia, leucopenia, neutropenia, and thrombocytopenia. Haematological manifestations of TB can be due to the direct effect of the infectious process, or it may be a consequence of antitubercular treatment. Normocytic normochromic anaemia or anaemia of chronic disease and raised ESR are the most common haematologic abnormality in TB.[2] Thrombocytosis and thrombocytopenia both are seen in TB [Figure 1]. Thrombocytosis is seen in pulmonary TB. Thrombocytopenia was commonly seen in disseminated TB or miliary TB. Thrombocytopenia in TB may occur due to defective platelet production in the context of pancytopenia due to bone marrow infiltration, histiophagocytosis, thrombotic thrombocytopenic purpura, disseminated intravascular coagulation, immune-mediated platelet destruction, or as an adverse effect of therapy with rifampicin and isoniazid.[4] Mycobacterium TB may share antigen with platelet, leading to antiplatelet antibody formation. Specific HLA presentation of TB could also lead to antiplatelet immunity response in some patients. In cases of TB associated with ITP, recurrence of thrombocytopenia is frequent in the first 2 months, and patients may benefit from close observation leading to a continuation of ITP-specific therapy.
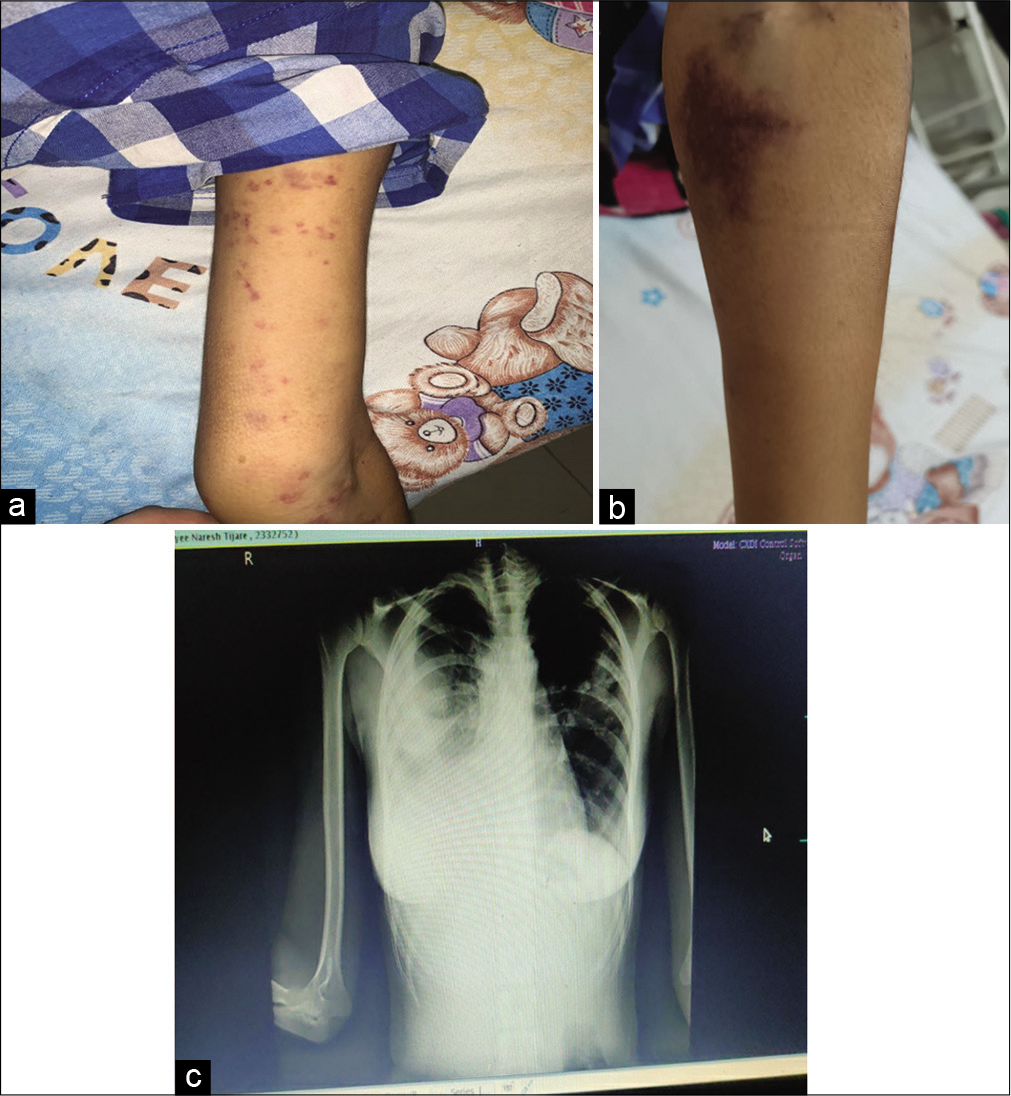
- (a) Petechiae on arm. (b) Ecchymotic patch on forearm. (c) X-ray suggestive of pleural effusion.
Acute kidney injury is a rare complication in patients on anti-TB therapy. Rifampin (RIF) is the most common anti-TB drug implicated in acute kidney injury (AKI) in patients on anti-TB therapy. The mechanism of RIF-induced AKI is not well established. Several studies suggest that it is either a type II or type III hypersensitivity reaction induced by RIF antigens in which anti-RIF antibodies form immune complexes that are deposited in renal vessels, the glomerular endothelium, and the interstitial area.[5] These reactions cause two different pathologic changes in the kidneys. The deposition of immune complexes in the vessels causes vascular constriction and tubular ischaemia, leading to acute tubular necrosis, whereas the deposition of immune complexes in the interstitial area leads to acute interstitial nephritis.[5]
Acute kidney injury in a patient with TB can also be a presentation of renal TB. Urogenital TB represents 27% of extrapulmonary TB cases. It is the third most frequent form of extrapulmonary TB after pleural TB and lymphatic TB. It occurs by haematologic dissemination of pulmonary TB in almost all cases. The development of immunosuppressive therapies is also responsible for the increase in the number of extrapulmonary TB cases. Early granulomatous kidney disease may present as proteinuria, pyuria, and loss of kidney function.[6] Isolated haematuria is another possible manifestation of renal TB. Urinary symptoms suggestive of urinary tract infection, accompanied by pyuria and haematuria with no bacterial growth, suggest urogenital TB.[7]
TB leads to a hypercoagulable state by increasing plasma fibrinogen level, impairment of fibrinolysis coupled with decreased levels of antithrombin III, and reactive thrombocytosis.[8] This hypercoagulative state could possibly lead to pulmonary thromboembolism and contribute to sudden death in patients with TB.[9] TB-related sudden deaths (TBRSDs) are a rare outcome of TB and mostly occur after initiation of antitubercular treatment.[10] The possible causes of TBRSD include tuberculous bronchopneumonia, massive haemoptysis, TB myocarditis, and adrenal insufficiency secondary to TB adrenalitis.[10,11] Our case highlights rare important complications of TB, and despite the development of specific chemotherapeutic agents for TB, TBRSD may affect patients receiving treatment that needs further evaluation.
Declaration of patient consent
Patient’s consent not required as patients identity is not disclosed or compromised.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
- Global Tuberculosis Report. 2019. Available form: https://www.apps.who.int/iris/bitstream/handle/10665/329368/9789241565714-eng.pdf?ua=1 [Last accessed on 2021 Dec 19]
- [Google Scholar]
- The prevalence and evolution of anemia associated with tuberculosis. J Korean Med Sci. 2006;21:1028-32.
- [CrossRef] [PubMed] [Google Scholar]
- Guide to drug dosage in renal failure. Clin Pharmacokinet. 1988;15:326-54.
- [CrossRef] [PubMed] [Google Scholar]
- Immune thrombocytopenic purpura. N Engl J Med. 2002;346:995-1008.
- [CrossRef] [PubMed] [Google Scholar]
- Acute renal failure due to rifampicin: A study of 25 patients. Am J kidney Dis. 2002;14:690-6.
- [CrossRef] [PubMed] [Google Scholar]
- Tuberculosis and the kidney. J Am Soc Nephrol. 2001;12:1307-14.
- [CrossRef] [PubMed] [Google Scholar]
- Deep venous thrombosis associated with tuberculosis. Blood Coagul Fibrinolysis. 2007;18:377-80.
- [CrossRef] [PubMed] [Google Scholar]
- Hemostatic changes in active pulmonary tuberculosis. Int J Tuberc Lung Dis. 2002;6:927-32.
- [CrossRef] [PubMed] [Google Scholar]
- Tuberculosis and sudden death: A case report and review. Heart Lung. 2001;30:388-91.
- [CrossRef] [PubMed] [Google Scholar]
- Tuberculous myocarditis presenting as sudden cardiac death. Forensic Sci Int. 1992;57:45-50.
- [CrossRef] [Google Scholar]






